Introduction
The majority of Australia is classified as ‘Very Remote’ by the Australian Standard Geographical Classification System, with geographical isolation, unforgiving terrain and weather conditions making many parts of the country difficult to access1. Despite the documented access concerns for isolated regions of Australia, 28% of the population still reside in regional, remote or very remote areas, with an 11% increase in population in these areas from 2011 to 20212,3. As rurality increases, life expectancy decreases4. Lack of access to appropriate primary care services, lower socioeconomic status and higher rates of smoking and alcohol consumption lead rural and remote Australians to experience greater negative health outcomes compared to their metropolitan counterparts4.
A lack of appropriate and sustainable resources – such as workforce and supplies, infrastructure (including unreliable internet connectivity) and funding and governance – impacts the sustainability and feasibility of healthcare delivery in isolated areas4-6. Approaches to overcome service delivery concerns have included implementing mobile locum services, fly-in-fly-out medical practitioners and telehealth models of care with diverse implementation and incomes, yet promising success7-9. Current literature highlights several potential models of care, barriers and enablers to implementing these models and workforce options to ensure the sustainability and feasibility of any healthcare service implemented in isolated Australian regions. Literature suggests that a telehealth model or mobile model of care may be most appropriate for these regions, due to barriers in cost-effective, appropriate and timely services7,10-13. Although telehealth has been highlighted as potentially the most feasible and sustainable model of service delivery in isolated regions, the rural ‘eHealth paradox’ as outlined by Liaw and Humphreys14 suggests that regions that may benefit most from telehealth solutions are the least likely to have infrastructure and resources to support the model.
Lack of appropriate health service delivery has been a key topic for communities in Far East Gippsland. This region borders with New South Wales, at the easternmost tip of Victoria, Australia15. Impacted by devastating bushfires and the ongoing impacts of COVID-19, many communities in the region remain isolated from the rest of the state. The Errinundra to Snowy Sub District is classified as a subdistrict of the Orbost district in the East Gippsland Shire, made up of nine communities and hosting a population of approximately 338 people16. The area is best known today for its livestock and plantation farming opportunities, with large uninterrupted land mass and rolling hills. Previously, the area was known for gold and silver mining, then later a booming timber industry, which is no longer in operation16. Today, the Errinundra to Snowy Sub District has a few shops and services including the Country Fire Authority, Australia Post service, Neighbourhood House services and town halls in the smaller localities. One larger locality also has accommodation, a general store, a pub, one primary school and one Multi-Purpose Service for health needs. The subdistrict is experiencing an ageing population, with 75% of the population aged between 50 and 69 years. The population is also facing potential decline, with a recent community survey suggesting that approximately 15% of the population wouldn’t stay or were unsure if they would remain in the district due to safety of roads and inability to access employment. Furthermore, only one in five residents believed healthcare services were adequate in the subdistrict16. Findings prompted further investigation and research into needs assessments and service equity projects within the subdistrict to increase awareness of lack of healthcare access, prompting policymakers to renew focus in the area after COVID-19 and the Black Summer bushfires.
The Black Summer bushfires in Victoria and New South Wales occurred between August 2019 and March 2020, burning a total of 19 million hectares, destroying over 3000 homes and displacing many more families. Thirty-three people lost their lives, and it was estimated that over a billion wildlife fatalities occurred. The Errinundra to Snowy Sub District was significantly impacted by the bushfires, with many losing their homes and livelihoods17.
This article provides a needs assessment of healthcare services in the Errinundra to Snowy Sub District after COVID-19 and the Black Summer bushfires. The project aimed to investigate the current healthcare services available to residents, as well as highlighting service strengths and gaps. Through investigation of current needs and available services, this study provides suggested feasible and sustainable services as suggested by the people that live there. As our healthcare landscape continues to adapt to the COVID-19 pandemic, this research is a timely investigation into the care needs of isolated Australian communities.
Methods
Aim
The aim of this research was to undertake a needs assessment of healthcare services in Far East Gippsland communities. Through this needs assessment, an understanding of the barriers and enablers to healthcare delivery could be ascertained. By gaining an understanding of the healthcare needs of individuals living in Far East Gippsland communities, suggestions could be made on the most feasible and sustainable healthcare model to be implemented in isolated Australian communities. The research questions that guided the research were as follows:
- What are the current healthcare facilities and services available in remote Far East Gippsland communities?
- What are the barriers and enablers to access and facilitation of healthcare services in Far East Gippsland?
- What are the most feasible and sustainable healthcare models that could be implemented in isolated Australian communities to promote access and facilitation of healthcare delivery?
Design
The research project employed a mixed-methods design. This was determined as the most appropriate method due to the multiple research objectives of the project. The incorporation of qualitative data added depth to the quantitative data, ensuring that voices of community members were adequately represented in the needs assessment.
Population
The study population consisted of community members of Far East Gippsland. Community members were those who defined Far East Gippsland as their main place of residence, some living in the area for several generations, while others moved to the area before and after the Black Summer bushfires for a change in lifestyle.
Recruitment
Participants were invited to complete a needs assessment survey in the form of a paper questionnaire. This questionnaire was delivered to Far East Gippsland communities by the lead researcher. The questionnaire was then distributed to each street address in the district by a local community group, with a confidential reply-paid envelope provided by the research team. This distribution method ensured quick delivery of surveys in a time-restricted project, guided by a group who understood the geography and context of the subregion. On completion of surveys, community member participants were given the choice to opt in to an in-depth individual interview.
Data collection procedure
Data for this project were collected using a mixed-methods approach. Quantitative data were collected using community surveys, while qualitative data were collected using semi-structured, in-depth interviews with community members via virtual meeting software Microsoft Teams.
Quantitative data
A community survey was distributed to Far East Gippsland community members during May 2022, with the aim of gathering information on the access, use and preferences of health care by consumers in the region. The survey was co-designed in collaboration with the research team and the community recovery committee in the subdistrict to ensure it was place-based, used language that was appropriate for the community and was sensitive to the community’s needs.
The community survey hosted a number of multiple-choice, Likert scale and open-ended questions. A total of 55 responses were received, with the majority of surveys returned as the paper-based form.
Qualitative data
Semi-structured in-depth interviews were undertaken with 11 community members residing within the subregion. A semi-structured design allowed participants to elaborate on their own personal experiences. Community members who opted to take part in the individual interview were asked a series of questions surrounding their use and access to healthcare services, the barriers and enablers to achieving this care and their future recommendations for health care in the subregion. Interviews with community members had a duration of between 15 and 41 minutes.
Data analysis
Quantitative data analysis was undertaken using descriptive statistics. This process involved collation of data from Qualtrics software v April 2022 (Qualtrics; https://www.qualtrics.com), reviewing characteristics such as frequency, tendency and variance of data distribution in order to summarise and report findings18.
Qualitative analysis was undertaken using a thematic analysis approach, using the Braun and Clarke19 method. In this six-step approach, the research team becomes familiar with the data set; generates initial codes based on content; searches for themes within the content; reviews themes as a collective to reduce individual biases, and define and name identified themes; then produces a report of findings.
Ethics approval
Ethics approval to undertake the research project was granted by the Federation University Human Research Ethics Committee (approval number A22-032) prior to data collection and analysis. Consent to participate in the project was achieved through signed informed consent and verbal consent given during in-depth interviews prior to the collection of data. All data were de-identified to protect the anonymity of participants. Due to the very small population in the Far East Gippsland region, participant anonymity was maintained by avoiding use of participant numbers and extensive demographic details beyond age, sex and locality. This was done to ensure those respondents who held specific roles or information within the community could not be identified through quote excerpts.
Results
Quantitative – community survey
Demographics
A total of 55 people returned the community survey, which was a 16.27% response rate. Of the 51 respondents to the question regarding gender, 45% (n=23) were female, 43% (n=22) male and the remaining 12% (n=6) preferred not to say. Respondents ranged in age from 20 to ≥80 years, with the majority (44%, n=22) aged 61–70 years. A total of 85% of the population lived in remote regions of Far East Gippsland in Victoria. A total of 28% (n=14) of people identified that they lived alone.
Accessing health care
A total of 53 participants answered a question regarding how long they would travel to see a doctor. Multiple participants (40%, n=21) identified that they spent an average of 2–3 hours travelling to see a GP. Responses to this question ranged from spending 1–2 hours (25%, n=13) or 3–4 hours (19%, n=10), with a smaller proportion spending 4–5 hours (11%, n=6) or ≥6 hours (6%, n=3) travelling. Of significance, none of the participants spent less than 1 hour travelling to their GP.
Wait times for appointments to see a GP were identified as extended. Of the 52 respondents for this question, 70% (n=36) of respondents identified that they had to wait 1–3 weeks, with 3% (n=2) reporting wait times of 3–4 weeks and 12% (n=6) identifying wait times of 5 weeks or more. A total of 15% of respondents stated they waited less than 1 week to see a GP (n=8).
A total of 81% (n=42) of participants reported that they had delayed seeking medical attention. Respondents were asked to expand on their response to this question, with reasons for this predominantly due to long distances or the time needed to get to and from an appointment (n=33). Other participants commented on the expense involved being too much (n=7), with these costs associated with missing work, fuel and accommodation.
Survey participants were asked how many times they were required to seek urgent healthcare services in the previous 3 years, including calling an ambulance, admission to hospital or presentation at an emergency department. A total of 50 participants answered this question. Most participants reported that they required these services one to three times (44%, n=22) in the previous 3 years, or less than once (did not attend) (38%, n=19) in the previous 3 years. Other responses included needing urgent services three or four times (8%, n=4), five or more times (6%, n=3) and unsure (4%, n=2).
When responding to how often participants required non-urgent healthcare services in the previous 3 years, 52 participants answered this question, with the majority reporting on average requiring services five or more times (56%, n=29). Such services included immunisation, health checks, specialist appointments, wound care, injury treatments or mild-to-medium illness treatments.
Participants were asked how many times in the previous 3 years they were too unwell to travel to seek medical attention due to illness or injury, with examples including vomiting, injured leg or other illnesses. Of the 53 respondents for this question, a total of 43% (n=23) reported that this occurred less than once (did not occur) and a further 42% (n=22) identified it occurred one to three times. Other responses included three or four times (11%, n=6), five or more times (2%, n=1) and unsure (2%, n=1). When identifying how they accessed healthcare services if they were too unwell to travel, some participants supplied free-text answers, most reporting that they relied on their partner, relatives, friends or neighbours (n=15). Others reported that they called for an ambulance (n=7) or made use of phone advice from a nurse, pharmacist or doctor (n=6).
Telephone and telehealth appointments
Participants were asked if they had used a telephone to access medical appointments. A total of 53 respondents answered this question, and the use of telephone and telehealth appointments was low, with 51% (n=27) ‘occasionally’ using telephone appointments. Interestingly 30% (n=16) of participants reported that they had ‘never’ used telehealth appointments. Only 10 respondents (19%) stated they used the telephone for appointments ‘often’. Participants were then asked if they had used ‘video meeting/telehealth’ to access medical appointments, with 77% (n=41) having never used this service. In free-text responses, reasons for not using telephone or telehealth were identified as not having the correct hardware to use such services, or that their phone or internet coverage was poor, meaning they were unable to use these services (n=8). Of concern, some commented that they were not aware of such services or were not offered them at all (n=6).
Experience with telephone, video or telehealth appointments
Part of the survey asked participants to comment on their experiences of using telephone, video or telehealth appointment services for their medical appointments, with almost all commenting positively in relation to the reduced travel time. Respondents identified that telehealth saved them time as well as money due to the associated costs of fuel and/or accommodation (n=6). One participant commented that they ‘didn't need to travel for simple results and uncomplicated health issues’.
Negative aspects of these services were also reported: it was often mentioned that the telephone service in the area was of a poor quality and there were issues with internet connections (n=7). One participant identified difficulty in explaining symptoms: ‘I found it hard to explain my symptoms over the phone. Would have been so much easier if I could have showed him’.
Types of health care needed
As part of the solution focus for the survey, participants were asked in an open-ended question format to state the types of healthcare service providers they needed. It was predominantly reported that GP services (n=32), followed by pharmacists (n=20), nurses (n=18) and dentists (n=16), were needed.
Participants were asked to rank a series of statements about what they deemed important aspects of health care (Fig1). Participants ranked the majority of the statements as ‘important’, with only 10% or less of particular elements of healthcare provision given an ‘unimportant’ ranking. Responses demonstrated access to healthcare and wellbeing management as a major priority for community members living in Far East Gippsland. The top statements ranked by the participants were ‘wound care services are available’, ‘a health professional is available in person’ and ‘the healthcare service is within 1 hour of my home each way’.
When assessing the preferences for delivery of health care, participants were asked to rank a number of options for their most preferred to least preferred method of accessing available care in their region. The six ranking options included two travelling options, two telehealth options and two in-home/in-community options for accessing care. Of the 49 respondents who answered this question, the majority (53%, n=26) identified their first choice as ‘travelling to a town of my choice to see a doctor in person at a clinic’. Their second choice (16%, n=8) was ‘access to a doctor via telehealth using an online meeting (like a Zoom or Teams meeting) at a community facility with the help of a nurse or other health professional’. The least popular choice was 'travel fo a large hospital to receive care' (39%, n=19).
Participants were then asked about their ‘ideal/suggested’ healthcare service delivery preferences for the region, which included five options such as telehealth at home or at a community facility, travelling and having care located within their localities. Of the 52 respondents for this question, the majority of participants (67%, n=35) stated ideally they would have a ‘physical GP on site at a clinic close by to them’ followed by the availability of ‘telehealth services from a community facility’ (17%, n=9). Other responses included ‘visit by nurse to home’ (8%, n=4), ‘telehealth from home’ (4%, n=2) and ‘travel to a hospital to receive care’ (4%, n=2).When asked about the ideal frequency of the preferred service delivery, 48% (n=25) of participants said ‘weekly’ and 25% (n=13) said ‘fortnightly’. Other frequencies included monthly or longer (28%, n=14).
Participants provided suggestions in an open-ended question about what would improve their healthcare experience in the subregion. Answers were related to the inclusion of a health professional stationed in the area, for example, a GP (n=10), a nurse/bush nurse or health professional (n=7), or an allied health professional (n=2).One participant commented that what was needed was ‘A regular nurse who is able to liaise and connect us with other services via outreach and visits of specialists. More government support to remote regional area instead of the slow stripping away of services’.
Participants also commented that they would prefer if a GP was also located in the area, the service was maintained and incentives were in place to encourage GPs to stay in the area ‘for years and not months’. One participant commented that ‘A regular visit by a GP at a community facility would be ideal to cover non urgent medical conditions like prescriptions and referrals’.
Isolated community members could see the benefit in using telehealth services to increase their access to healthcare services, yet it was identified that infrastructure and digital literacy may provide a barrier in appropriate facilitation. A desire to provide solutions to complex problems was evident in the comments of community member respondents, suggesting that their motivation to source a feasible and sustainable model of care to remain living and thriving in their local communities was high.
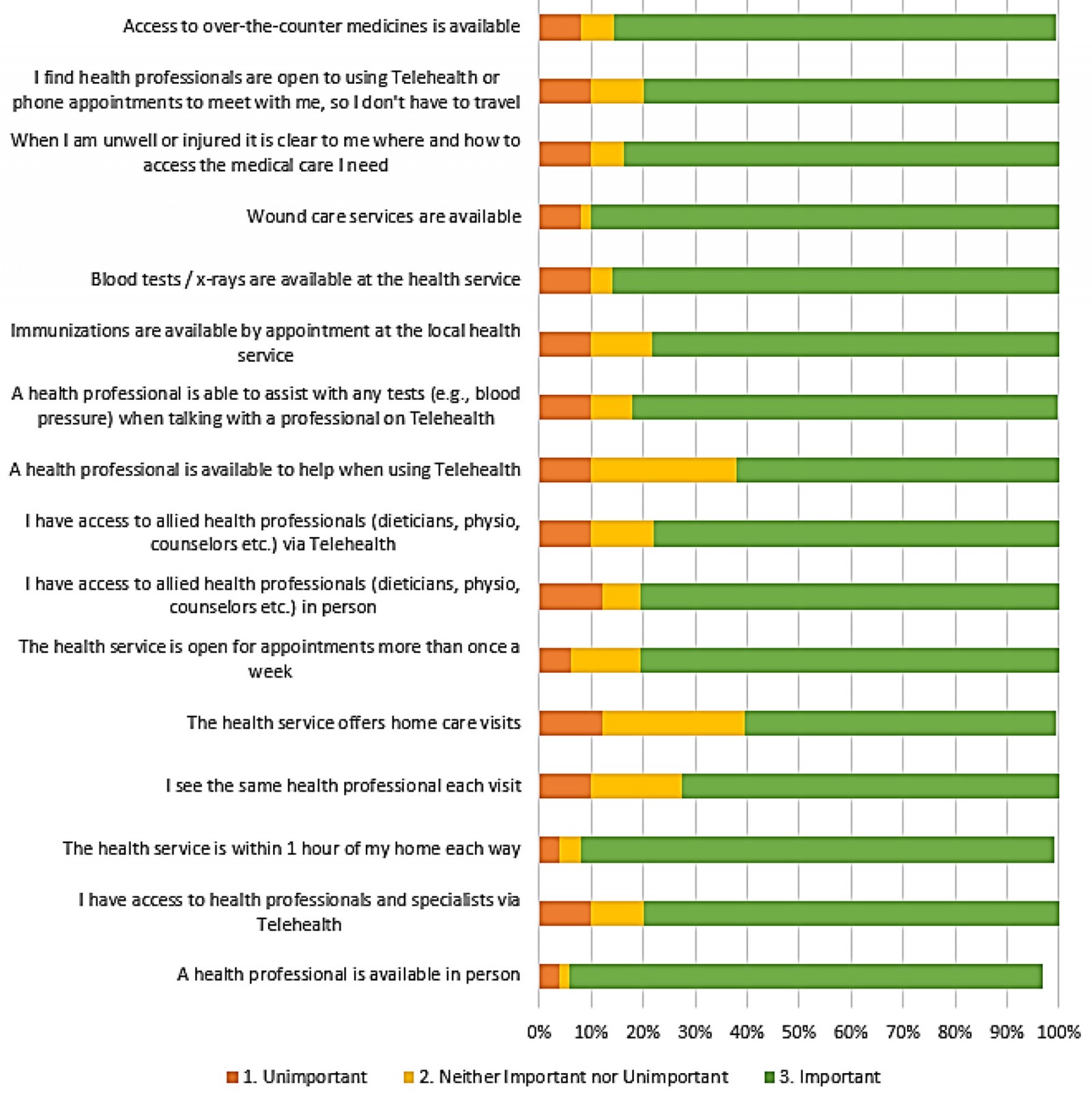 Figure 1: Importance of healthcare services to survey respondents in the Errinundra to Snowy Sub District in Far East Gippsland, Victoria, Australia.
Figure 1: Importance of healthcare services to survey respondents in the Errinundra to Snowy Sub District in Far East Gippsland, Victoria, Australia.
Qualitative – interviews with community members
Five themes emerged from semi-structured interviews of 11 participants from remote communities in Far East Gippsland. The interviews were transcribed verbatim and analysed using the Braun and Clarke19 six-step thematic analysis technique. The findings are presented here under the five theme headings.
Accessing health care
Participants noted the complexities of cross-border healthcare delivery, identifying challenges to access. There was currently no cross-border arrangement available to bridge the gap of service delivery between states in Australia, leaving residents having to travel long distances to appropriate specialists, often resulting in the creation of informal arrangements so care could be provided. A possible solution to address the issues of accessing healthcare services in cross-border regions was the use of mobile health services, including vehicles or buses that have essential care items on board that can access remote regions:
… I'm not suggesting that we should have bloody facilities for an MRI here ... You know, that's kind of ridiculous. But there's got to be some better cross border arrangements, there's got to be better mobile health facilities.
Aging rural populations added another layer of complexity to the issue, with some residents unable to access mobile services due to lack of personal transport and capacity, despite the services coming to a local facility such as the local community centre. Furthermore, many elderly residents were not linked into the community notice boards and were unaware of the timing of visiting specialists:
… Well, if we get services to come to our local halls, we still need to get the local people to the halls … quite a few of these elderly people don't have vehicles anymore. They can't drive. We have to organise a little local minibus to pick them up and bring them to these services … A lot of the times they just, don't hear about the service until they've been and gone, and if they do hear about, they say ‘well I can't go there because the neighbour who drives me is not available at that time’.
Many rural and remote residents travelled over 200 km to access healthcare services, such as a visit to a GP, which was often on poorly maintained country roads and resulted in a loss of a day’s income, which had wider implications for the maintenance of a rural farming property:
When you travel from here, we live on a farm where I've got animals. It wrecks your whole day … not only the cost of petrol ... You have to work when you live on the land.
Despite these issues, participants noted the quality of the current mobile health services in the region while identifying the need for a higher frequency of visits.
Health services that work well
A number of visiting services were identified as beneficial from both a health and social perspective for communities. Multiple services visited on a single day, creating a community event atmosphere with the ability of residents to access a variety of services at one time:
… they get the medical ones from [town] to come up. Doctors and skin specialists, and it was just like a big meeting thing. The Shire come and it's a good day, really. It's just a full day and they have lunch and everything there.
Allied health services were provided to the region on a visiting basis. The Royal Flying Doctor Service provided dental and optical health care, which was a much-needed and appreciated service to the area that participants would like to see extended. The service was well utilised, with participants identifying that appointments were booked well in advance:
The Royal Flying Doctor Service comes around and does a dental clinic twice a year. They were only here about a month ago, but … daily have about 20 appointments over the four-day period that they're here, and they're booked months in advance.
Telehealth and virtual meeting software increased the accessibility of some health services; participants identified this service as a potential future solution with expansion into allied health services.
Although almost all participants identified some positives about the current health services, and the value they placed on these was evident, participants also realised the limitations of these services and the implications.
Limitations of health service delivery
There were several identified limitations to the current health service delivery for these rural and remote communities, with many feeling that they were receiving minimal or substandard health care:
I've got no faith whatsoever, no faith whatsoever in the healthcare system in East Gippsland, none, zero.
The cross-border issues also impacted emergency services, with confusion arising about responsibility for responses to accidents or incidents in rural and remote communities. This could have led to additional stress, but also importantly had the potential to result in negative and life-threatening time delays for those in need of emergency care:
… we've had some pretty bad accidents up there in the last two years, and it's been a fight between the ambulance in Victoria and the ambulance in New South Wales. And usually, we just get people helicoptered out because they're usually pretty badly injured. So it's a real concern …
Shortages and lack of staff available to work in local health care resulted in patients accessing alternative services. Some participants cited this as a reason why they didn’t access the closest Multi-Purpose Service as they felt it delayed treatment, therefore they chose to bypass it in favour of a larger service that was adequately staffed:
… we don’t even bother using the [town health service] because they don’t have a doctor there. They only have a few nurses, and if you go there, all they ever do is refer you on to [town] or you know, just say you need to go.
It was evident from the interviews that participants were aware of the difficulties of getting health services to the area due to the remoteness; however, all participants identified the need to be provided with basic services to meet their health needs.
Community solutions for better health care
Although the participants were able to highlight the various limitations and complexities involved in receiving health care in remote communities, they remained solution focused and positive, especially about bush nurses and the existing healthcare providers who go ‘above and beyond’. Having a nurse or doctor close by in times of emergency provided comfort for families:
A [person] died out here, way further out in the bush ... and there’s no [services] to fly people in, obviously, which they probably would have to do anyway. But I think that you know the benefit of [the] family and that would have been nice if there was a nurse or a doctor or someone closer that could have come out.
A potentially viable option for the isolated communities included improving the telecommunications capacity for telehealth. Telehealth had the potential to accommodate a variety of services such a medical appointment, specialist care and allied health consultations:
… we have the facilities, both at our neighbourhood centre and at our community hall, to do videoconferencing … we’re not particularly computer savvy – but if we had opportunities to have face to face videoconferencing health things, I think that could be handy.
It was also important to have continuity of care to ensure holistic health care was provided. Having a healthcare professional who knew participants’ health status and medical history could potentially foster trust in the delivery of care, facilitating a connection between patient and practitioner:
… it would be good when there would be a GP coming regularly. Hopefully the same one and not every time a different one. I think it’s important that you have your own GP who knows you and knows your lifestyle maybe. Knows what your ailments, what you had before happening to you. Because all those things I think are related to each other in health.
The participants provided several healthcare service delivery suggestions based on their individual and community health needs, utilising and enhancing existing infrastructure.
Community informing policy
Participants identified the need to be heard by those in a position to generate health policy, in addition to being able to influence policy that related to rural and remote areas. Walking in the shoes of the community by spending time understanding the complexities, issues and restrictions to accessing adequate health care was deemed vital:
I guess it might sound rude advice but for [policymakers] to spend time in the community. Have them or their family or loved ones get crook, get sick, and go through the throes of what's involved in trying to get medical services. Then they might be thinking out of the metropolitan area a bit more.
Participants welcomed the development of healthcare models that addressed the complexities of accessibility and rurality such as a ‘bush nurse’ arrangement, ‘over the phone’ or ‘Zoom’ virtual meeting software options when accessing care. Adequate health care was cited as one of the major reasons why residents either don’t move to the area or leave the area, especially those with chronic conditions or advanced age:
… lots of old people that just, yeah, they moved away. Because they can't live here with the health issues, they move to towns where there’s more support which is really sad that you have to leave your family home, you know, when you get old and moving into town because there's no services here. Pretty sad.
Finally, equitable access to healthcare services was highlighted by community members. Access to safe and appropriate services was outlined as a basic human right for all Australians, regardless of where they live:
… it doesn't matter where you live in Australia, you have as much right to services as anybody else, whether they be health or education or police or whatever they are. And to keep on saying your statistics or your numbers of people in your community or whatever they are don't warrant that service, is untrue. Because a person is a person no matter where they live.
Community members needed a mechanism in which to influence policymakers to ensure that government agencies continue to explore health service access solutions in isolated regions in Victoria. Participants outlined wanting to have a voice to policymakers, for policymakers to visit the region to better understand the geographical and socioeconomic intricacies of Far East Gippsland.
Discussion
This study presents findings on current healthcare access and use for rural and remote Australians living in a subdistrict of Far East Gippsland. By investigating the current healthcare facilities and services available, in addition to identifying the barriers and enablers to access and facilitation of these services, determination of a feasible and sustainable healthcare model may be realised.
Current Australian literature supports the implementation of safe and equitable telehealth and mobile services in isolated regions, potentially bridging the gap in service provision7,10-13. Telehealth can support face-to-face care in isolated communities by providing virtual routine examinations, prescription refills and supporting care in uncomplicated presentations, providing reassurance to patients and reducing disruption to daily living13. Findings from this study support literature, with participants recognising the innovation that may be realised with implementation of novel technologies. Participants were supportive of mobile health care, stating that these services provided regularity and complete care during designated times of year. As outlined by Lesjak et al in a study implementing a mobile screening service for disease prevention7, the service achieved good levels of engagement and was proven feasible to organise and operate within isolated Australian regions. Beyond physical transport mobile health services, some providers in Australia have had success in taking their service by plane or car and setting up equipment transiently in existing community buildings20,21. These outreach clinics may provide more place-based, timely care to communities that otherwise do not require or cannot facilitate a permanent health service. Some community members in this study outlined how mobile and outreach health care provided them with enough care that was tailored to their lifestyle and healthcare needs. These findings highlight how mobile, outreach and telehealth models of care may meet several of the healthcare access desires of the Far East Gippsland community, whose values surrounded receiving care within 1 hour of their home, knowing who to contact and where to go when in need, and receiving care from someone in person who could provide continuity of care.
Participants of this study acknowledged that their digital literacy skills were lacking, increasing barriers to access and use of digital technologies. Digital literacy coupled with lack of available resources and connectivity in regard to digital services increases the divide in appropriate care provision14. Contributing factors to the ‘rural eHealth paradox’ include fragmented and inadequate policies and legislation around the implementation of e-health, inadequate infrastructure, models and support coupled with lack of confidence in e-health solutions from both the provider and consumer14. With the global impact of the COVID-19 pandemic having changed the digital environment of care delivery, the need to prioritise the development of feasible and sustainable digital infrastructure is crucial. The use of digital health care during the pandemic ensured that care could be delivered safely, maintaining social distancing and prevention of transmission to vulnerable populations22. There remains a lack of appropriate literature in the peri-COVID-19 era on the implementation of telehealth services in regional, rural and remote Australia. This lack of evidence is more apparent with the impact of border restrictions during the pandemic for isolated communities within Far East Gippsland. Participants in this study highlighted the difficulties in accessing cross-border health care due to closures and restrictions, although this was outlined as the safest and most reliable route of travel to appropriate care. The untapped resource of telehealth care in rural and remote regions may have provided more timely care during these instances of COVID-19 lockdowns, and it requires further investigation and investment to achieve the same digital connectivity momentum as metropolitan centres. A gap in the literature remains on successful telehealth pilot studies that can be scaled and translated beyond their original location.
A strong theme of not wanting to be forgotten by policymakers was evident in responses from participants. For people of influence to experience the lives and perspectives of community members was outlined as vital in addressing needs from a place-based perspective. Although investigation into improving the health and wellbeing of isolated Australians is not a novel idea, there remain diminished services to those vulnerable populations and a lack of timely inquiry from a peri-COVID-19 perspective23. The 2019–2020 bushfires in Victoria and New South Wales significantly exacerbated these diminished services, with community members losing assets, infrastructure and capacity to receive timely care20. This added complexity to the region and requires a timely and compassionate response from policymakers to ensure regeneration of services within Far East Gippsland.
Global positioning and implications
Findings from this study may be of significance in diverse global settings with similar geography and rurality. With the emergence of COVID-19 and the need for virtual, contactless healthcare provision, greater emphasis on connecting rural and remote communities through digital models is required. Global telehealth and digital health discussion by Ramnath24 suggests the need for design thinking, using creative and innovative solutions that suit the specific needs of the community it intends to serve. The needs assessment outlined in this study from Far East Gippsland has demonstrated the difficulties juxtaposed with benefits of virtual health care, suggesting that innovative telemedicine tailored to the holistic needs of an isolated community is required to increase understanding, uptake and beneficial outcomes for its users. Review findings from Africa during the COVID-19 pandemic saw telemedicine as a beneficial tool for health service provision, education and connection25. The authors’ proposal of policy frameworks that support telemedicine use are of great significance to the present study and the Australian context, with similar contextual barriers faced including geographical isolation, digital barriers and lack of supportive existing models24. Modelling of various successful global telehealth strategies may provide policymakers with a supportive framework that can be tailored to the Australian context.
Limitations
Due to a lack of reliable telecommunication infrastructure, undertaking virtual interviews provided challenges. Varied weather conditions and unreliable telephone reception meant that some participants could not be reached. This was a foreseen potential barrier to data collection; however, the remoteness of communities and inability to undertake face-to-face interviews due to privacy concerns in small communities meant that virtual interviews were the most appropriate mode of collection. Furthermore, due to the short timeframe for project completion, participants were given approximately 3 weeks to complete the written survey. Due to the remoteness of participants and access to mail delivery services, this may have restricted participation. Despite this, an appropriate sample of 16.27% of the population was achieved, validating the survey findings.
Conclusion
Achieving safe and equitable health care is a basic human right for all people. Individuals and families living in rural and remote Australia have decreased access to care that is appropriate for their needs, ultimately increasing morbidity and mortality. Access, use and facilitation of appropriate place-based health care within isolated Australia has the potential to increase wellbeing and enables residents to remain in regions that hold long historical and familial connections. Incorporating innovative technologies, removing access barriers and implementing models of care that have been evaluated across other isolated regions of Australia and globally offers an opportunity to adapt existing models to conform to a post-COVID world.
Funding
This research forms part of a funded research project by the CERC in partnership with the Deddick Valley Isolated Community Group Inc. No other specific grant from any funding agency in the public, commercial or not-for-profit sectors was received.
Conflicts of interest
The authors declare that they have no conflicts of interest.
Acknowledgements
The Collaborative Evaluation & Research Centre (CERC) acknowledges the Deddick Valley Isolated Community Group Inc. in their ongoing consultation and guidance throughout this collaborative research project.



